Orthorexia – The Not-So-Healthy Obsession with “Healthy” Eating

similar to those of OCD and Eating Disorders.
Orthorexia Nervosa (also simply known as Orthorexia) is a relatively new term within the psychological and medical fields. Simply defined, Orthorexia is an eating disorder in which an individual has an excessive and ultimately unhealthy obsession about maintaining a diet that is totally “healthy” and “pure”. Because of their extremely restrictive eating, individuals with Orthorexia are often severely underweight, and frequently lack the proper nourishment to perform basic daily activities. Like most cases involving an eating disorder, the outcome of Orthorexia can be severe malnutrition and a significant reduction of one’s quality of life.
Orthorexia has not yet been accepted as a formal diagnosis by the psychiatric community, and has not been defined within the Diagnostic and Statistical Manual (DSM-IV). However, since first being described by Dr. Steven Bratman in 1997, many health professionals have observed the often debilitating results of this condition.
Symptoms of Orthorexia
Like Obsessive Compulsive Disorder, Orthorexia can be conceptualized as a constellation of obsessive thoughts and compulsive behaviors. The most prominent obsession seen in Orthorexia is an excessive concern about the healthfulness of food. Those with Orthorexia often spend many hours of the day planning and obsessing about what foods they have eaten or will eat, the nutritional content of that food, and how that food has been grown, processed, and/or prepared. Individuals with Orthorexia may obsess about any number of nutritional aspects of food, including, but not limited to the following:
• Calories
• Sugar (especially “refined” sugar)
• High fructose corn syrup
• Fat
• Hydrogenated or partially hydrogenated fat (trans fats)
• Protein
• Carbohydrates
• Glycemic index
• Salt / sodium
• Fiber
• Gluten
• Dairy products
• Fatty acids
• Vitamin and mineral content of the food
• Whether or not a food is “whole” or “organic”
• Whether or not a food is sufficiently vegan, vegetarian, or macrobiotic
• Whether or not a food is genetically modified
The most obvious behavioral symptom of Orthorexia is the compulsive avoidance of foods that the sufferer deems unhealthy or impure. Individuals with Orthorexia may at first simply eliminate a few specific foods from their diet, but over time, their diets often become more and more restrictive. Eventually, they may eat only a select small number of foods that have been prepared in a manner that they have decided is “correct” or “pure”. At the same time, they may also purchase many expensive, “natural” or “organic” health food products and supplements that they perceive as more pure and/or healthy than traditional foods.
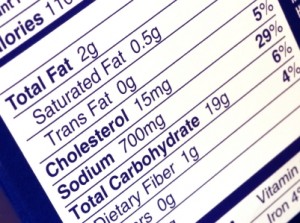
In addition to food avoidance, individuals with Orthorexia will often spend excessive amounts of time researching food issues related to the above concerns. This research may include many hours of internet searching, buying and reading an excessive amount of food, health, and nutrition related books, and near-constant examination of food labels when shopping for groceries at the market.
For individuals with Orthorexia, the obsessive concern with what goes into their bodies may also extend to other, non-food related health issues. Often, they have a disproportionate level of fear related to the possibility of exposure to what they perceive as pathogens in everyday products and in the environment. This may result in compulsive avoidance of certain soaps, shampoos, perfumes, and deodorants, as well as x-rays, vaccinations, or even mercury in dental fillings. They may broadly reject much of western medical science in favor of homeopathy, osteopathy, and other “complementary” and “alternative medicine” approaches.
It is also common for those with Orthorexia to spend much of their social time discussing food, and attempting to convince others of the “correct” way to eat. This may result in conflict with families and friends who do not agree with their views, and who take offense when the person with Orthorexia repeatedly criticizes their food choices. Likewise, those with Orthorexia may take offense when friends and family express their concerns about the health and dietary choices of the sufferer.
On a more internal, psychological level, those suffering with Orthorexia often experience significant guilt and shame when they do not maintain their purist dietary rules. They are usually extremely strict with themselves about their diet and their overall health, and are often overly judgmental towards themselves and their ability to control what they eat. Frequently, much of their self-esteem and sense of identity is rooted in their diet and in their success in satisfying their high levels of self-discipline.
Diagnosis and Relationship to Obsessive-Compulsive Disorder
While some see Orthorexia as an eating disorder, many mental health experts agree that it is best conceptualized as a hybrid of an eating disorder and Obsessive Compulsive Disorder (OCD). Like OCD, Orthorexia is defined by the individual’s obsessive thoughts (in this case, thoughts about certain foods being  dangerously unhealthy), and the compulsive behaviors done in an effort to minimize the anxiety caused by those obsessive thoughts (in this case, food avoidance, as well as the other behaviors noted above).
dangerously unhealthy), and the compulsive behaviors done in an effort to minimize the anxiety caused by those obsessive thoughts (in this case, food avoidance, as well as the other behaviors noted above).
The food avoidance seen in Orthorexia also has an obvious relationship to Anorexia. In fact, many with Orthorexia are eventually diagnosed with Anorexia as a result of weight loss related to their food avoidance. And some mental health clinicians see Orthorexia as a behavioral symptom of Anorexia in which the individual uses the issue of “healthfulness” as a justification for not eating.
It is also worth noting that some with Orthorexia will resort to purging behaviors similar to those seen in Bulimia in an effort to rid their bodies of impurities that they believe they may have ingested. Purging behaviors may include vomiting, use of laxatives and emetics, and use of colon cleansers to rid themselves of alleged toxins. Likewise, similar to those with Anorexia and Bulimia, individuals with Orthorexia often perform other compensatory behaviors such as compulsive exercising in an effort to make their bodies as perfect and pure as possible.
Symptoms of Orthorexia also overlap with those of other Obsessive Compulsive Spectrum Disorders. The excessive focus on “healthfulness” leads many to develop a distorted over-concern with their actual health, not unlike those with Hypochondria (also known as Health Anxiety). Likewise, many with Orthorexia have a distorted body image, much like those with Body Dysmorphic Disorder (BDD).
Because of the extreme restrictions commonly seen in this condition, it is often very difficult for those with Orthorexia to eat socially, or even be in social places at all. As result of trying to avoid being confronted about their food obsession, many with Orthorexia develop a pattern of social avoidance similar to that of Social Anxiety. The result is often a reduction in social interaction, and in some cases, a complete severing of friendships and relationships in order to maintain and protect their diet.
Finally, it is worth noting the overlap between phobias and Orthorexia. The two primary distinguishing features of phobias are the sufferer’s irrational fear of a specific object or event, and their subsequent efforts to avoid exposure to that object or event. Some conceptualize Orthorexia as essentially being a food phobia, in which the individual is terrified of being exposed to foods that they irrationally see as imminent threats to their well-being.
Click here to read part two of this series, which examines the treatment of Orthorexia utilizing Cognitive Behavioral Therapy.
•Kimberley Quinlan, MFT, is a licensed psychotherapist at the the OCD Center of Los Angeles, a private, outpatient clinic specializing in Cognitive-Behavioral Therapy (CBT) for the treatment of Obsessive-Compulsive Disorder (OCD) and related conditions, including Orthorexia. In addition to individual therapy, the center offers four weekly therapy groups, as well as online therapy, telephone therapy, and intensive outpatient treatment. To contact the OCD Center of Los Angeles, click here.





















































12 Comments
Hello, I found this article very interesting but at the same time it raised some questions for me.
I have OCD and I am also try to eat very healthy and avoid many of the items referenced on your list. Quite frankly, I don’t understand why in this case trying to eliminate obviously unhealthy and harmful ingredients from one’s diet would be considered a disorder. After all, isn’t this what the media and the nutrition professionals teach us to do?
Please explain.
Hello there Emily,
Thank you for your question. I completely understand your concerns.
The term Orthorexia does not automatically apply to anyone who is trying to eat a healthy diet or who is eliminating unhealthy foods from their lifestyle. The term is used to describe someone who is restricting their diet so much that they begin to become malnourished and their health is being threatened. This is usually due to severe restriction of specific types of foods. Commonly, people who suffer Orthorexia do not eat from all of the food groups and often don’t get enough calories. Basically, they eat “healthy” to a point that is “unhealthy”, both physically and psychologically.
Also, Orthorexia comes with time-consuming obsessions about food. Sometimes, the whole day is taken up obsessing over what foods will be eaten? And when? And how much?
I hope that helps differentiate between those who have Orthorexia and those who are just trying to have a healthy dietary lifestyle. I too try to prepare healthy nutritious meals for my family and my self, but like all things, this must be done in moderation. If eating becomes too extreme, there are often physical, emotional, and/or social consequences.
Please let me know if you have any additional questions.
Warmly,
Kimberley
I hardly eat at all, this describes me perfectly. I have almost stopped eating because I can’t find many foods that meet my standards. I know it is crazy but I can’t stop
Hello there Jill,
You are not alone. A lot of people feel there is no way to stop. Know that you are not alone and that you can get better.
Seeking professional treatment for Orthorexia will allow you to learn tools to help manage the discomfort of stepping out of the rules of this condition, and can provide you with the support you need to do this. I wish you all the luck. Don’t give up!
Warmly,
Kimberley
Hi, something I have encountered before as a pure o ocd sufferer that I am wondering if it’s similar to orthorexia – the idea however is not about food, but water. My brother has anxiety but did this as well and I have OCD. Obsessing over the taste of water and cleanliness of water, for a few months we both stopped drinking our water suddenly and switched to bottled water (which if your familiar with studies may not be cleaner anyway!) but something about the water became an anxiety for us both. However with me I think it may be related in some way to how ortharexia works or at least my OCD. We both no longer have this issue, but I have since met others with it (to my honest surprise). Often those I meet now do have a comorbid eating disorder, but not always. It doesn’t pear to be super common, yet it can obviously be very detrimental to ones health- especially if you are dehydrated chronically. In similar fashion I’ve also met people who will not drink water at all- a friend who would only drink soda for about four years. I was wondering if you had any thoughts or information on this (not that I’m asking for a diagnoses, just info, and what this is related to. Just anxiety?) regards, Risa.
Hello Risa,
Any thought can become an obsession when we give it a lot of value. And, each obsession becomes problematic when we respond to it as if it was a fact, even though we don’t want to or know that it doesn’t make sense. Or, in many cases, we respond because we couldn’t handle the discomfort if we didn’t respond.
Orthorexia is an obsession surrounding the healthfulness and purity of ones diet. While an obsession about the purity of water alone might not qualify one for a diagnosis for Orthorexia, the treatment of this obsession (and the compulsion to avoid tap water) would be treated using exactly the same tools. It would be important to gradually expose one to their fear and learn that they can tolerate the discomfort.
Lastly, there are many overlaps between OCD and Orthorexia. The most important thing would be that each person be assessed thoroughly before beginning treatment.
Warmly,
Kimberley
I’m in my twenties and I used to weigh 300lbs, which depression and a strange course of events lead me to lose around 100lbs of that weight in a very short amount of time. I lost this weight by no longer eating sugars, bye-bye soft drinks, and by starting to regularly drink chilled water. I thought I was being healthy but your words above really do describe me quite well. to an extent. I’ve maintained a 200lbs weight for the past 2 years now and was arguably feeling pretty good about my appearance until something happened that negatively altered the way I look. Now I feel like theres no point in eating “right” cos my appearance is all screwed up anyways. Now I have all these incredible urges to just raid the pantry and eat everything in there and I can’t shake the thoughts, they’re there 24/7, and my usually impenetrable will-power is finding it painfully difficult to fight these feelings off. I’m afraid that if I let myself eat whatever like I did before that I’m gonna end up overweight again. I’ve had Obsessive Compulsive tendencies all my life and I guess I’m just looking for some advice or opinions on my current situation. Thanks.
Hi there Ben,
While I applaud you for your healthy eating, it is important to note that some take healthy eating to an extreme.
I strongly encourage you to observe your thoughts and recognize that just because you have thoughts that foods must be “right”, doesn’t mean they must, in fact, be right. Similarly, just because you have thoughts that you will over-eat and gain weight, doesn’t make them facts either.
Taking this observational view can help you see that these are just fears, not realities. I also encourage you to find a therapist who specializes in treating Orthorexia to help you with appropriate exposures to help with these fears.
Wishing you all the luck.
Kimberley
Hi, thanks for the great article. I see it’s a few years old so you may not be taking replies now. I had a visit from worried friends who have drawn my attention to this and I realise it describes me well. I’m extremely low and unhappy and have been for some time – my healthy diet seemed to help give me some order but I realise I’ve taken this to extremes. I’m struggling to find balance and settle in life and have tried lots of therapies and supplements and visited my doc to a lot. The OCD and hyperchondria you describe seem to apply to me to! I’m not sure where to turn next but am considering life coaching and/or counselling – can’t decide whether it’s better to try and get to the root causes of this of just look forward. Any ideas please? Much appreciated.
Hi S,
Sorry for the delay in replying.
While I cannot provide a diagnosis via a blog comment, I can say that the symptoms you describe sound very much like Orthorexia. This condition is very similar to OCD, and the best solution is to find a therapist with experience treating Orthorexia with Cognitive Behavioral Therapy (CBT). I am confident that a life coach or a traditional talk therapist would be clueless with helping you to manage Orthorexia. In fact I would be stunned if they had even heard of it.
Hello. After reading this, I feel like my daughter may suffer from this. She is now 20 years old, has been vegetarian for 10 years, and severely restricts her diet. I never see her eat sugar. She buys sugar-free syrups for her coffee and tea, and low-carb, sugar-free ice cream, sugar-free soft drinks and sugar free jello snacks or fruit cups. She eats a lot of eggs, as a response to our request that she makes sure she eats enough protein, and she eats a lot of vegetables. These are the only things I see her eat. I recently brought back cupcakes from a visit to Washington DC from a famous bakery. She wouldn’t eat hers in front of me, but the next day I came home from work and half of it was still in the fridge. She claimed to have eaten the other half, but I don’t know if I honestly can believe she didn’t throw it away. She won’t eat carbs – buys low cal bread, no longer eats pasta (she grew up on Pastina, we are Italian.) Claims she “doesn’t like the texture.” She has developed amenorrhea twice. I am at my wits end. Her doctor (a slender woman herself) doesn’t seem to thin her ‘watching what she eats’ is a big deal. I don’t agree, do you?
Hi Julia,
I cannot provide a diagnosis via a third-party report on a blog. Also, the line between healthy eating and Orthorexia is not always easy to define. Generally speaking, they key distinction is whether the dietary choices are causing problems in the individuals’s life.
There is nothing innately wrong about eating a vegetarian diet that is low on sugar and processed carbohydrates. However, the fact that your daughter has twice developed amenorrhea is a strong indicator that something is seriously wrong. Many women with Orthorexia experience the loss of their period, and this is a genuine cause for alarm, as it indicates that her body is responding to a lack of nutrition.
Ideally, your daughter will be able to recognize that her extreme dietary choices are taking a negative toll on her. I encourage you to provide support and compassion, while at the same keeping an eye on her symptoms. If at any time she expresses concerns, take that as an opportunity to lead her towards help with a treatment provider who has experience treating Orthorexia.